Rilynn’s Journey
When Brittany and I were asked to write this letter, we had mixed feelings. Rilynn’s journey into this world has been an emotional roller coaster with breath taking highs and scream provoking lows. Not for a second in the broken road of life did I ever think I would have to ask the questions I did, nor hear the honest answers I received. Hold on to your safety harnesses, here is the compressed version of our experiences on the Rilynn Nicole German journey.
I credit the beginning to a fantastic doctor named Dr. Melissa Espisito at Shady Grove Fertility. She is the most sweet, pleasant and genuinely caring person. Brittany and I had been trying any and every method to conceive a child for approximately 18 months prior to being referred to Dr. Espisito through a friend. Her calm and personable approach to creating families took the sting out of those months when the phone call said, ”Sorry, you are not pregnant. We will see you Tuesday for your next appointment.” We didn’t want another appointment. We wanted a baby. After 2 years of those phone calls, Brittany underwent the Invetro Fertilization process of harvesting her eggs, collecting sperm samples and arranging their meeting in a pietri dish. We finally got the phone call we wanted, “Congratulations, you’re pregnant.” After a few weeks of monitoring, Dr. Espisito noticed that Rilynn was not growing as fast as she should be. Dr. Espisito referred us to to a High Risk OB name Dr. Wayne Kramer to monitor Rilynn and figure out the growth restriction. Dr. Kramer in Frederick, MD would scratch his head and say to Brittany every two weeks, “It’s okay kiddo.” We could tell something was wrong but he didn’t want to alarm Brittany. His kind and gentle approach to the growth restriction mystery would allow us to open up to Dr. Bringman at West Virginia University’s High Risk OB office in Morgantown, WV in June of this year. In the middle of this stressful journey, I, Bill German (Dad), took a job in the Deep Creek lake Area of Western Maryland. This meant I would be away from my pregnant wife during the week and would travel two and a half hours one way to see her on the weekends. Even in the middle of the night (during snow storms) when she was having a bad day. Brittany and I discussed this move with Dr. Kramer and he did the research for us on what we were going to need medically for Rilynn prior to, during and after birth. He suggested Children’s Hospital on the campus of West Virginia University. They are a state of the art teaching hospital with a highly regarded Neonatal Intensive Care Unit. Dr. Kramer made the phone call and transferred our records to the High Risk OB office at WVU. This is where we met Dr. Jay Bringman. Dr Bringman is a brilliant man. He has broad shoulders with a straightforward approach. He took on Rilynn’s mystery within minutes of speaking to us. After 4 days of waiting for the Amnio test to come back and worrying if the test would cause a miscarriage, we arrive for what we thought would be a “normal” OB visit. Although Wolf-Hirschorn Syndrome can be explained using very big words, Dr. Bringman chose to use a plain and simple explanation. Unfortunately, we did pick up on the “this is serious” look in his eyes. Then, it was a compassionate conversation with Dr. Obringer (Adult Geneticist). Dr. Obringer explained to us in plain English and in medical terms what Wolf-Hirshorn Syndrome is and how it would affect our lives forever.
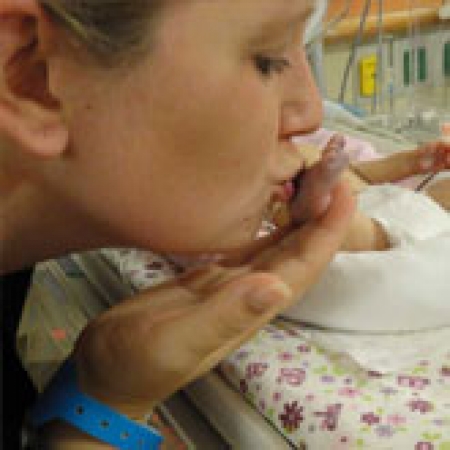
The prevalence of Wolf-Hirschhorn syndrome is estimated to be 1 in 50,000 births. For unknown reasons, Wolf-Hirschhorn syndrome occurs in about twice as many females as males.Wolf-Hirschhorn syndrome is a condition that affects many parts of the body.
The major features of this disorder include a characteristic facial appearance, delayed growth and development, intellectual disability, and seizures. Almost everyone with this disorder has distinctive facial features, including a broad, flat nasal bridge and a high forehead. This combination is described as a “Greek warrior helmet” appearance. The eyes are widely spaced and may be protruding. Other characteristic facial features include a shortened distance between the nose and upper lip (a short philtrum), a downturned mouth, a small chin (micrognathia), and poorly formed ears with small holes (pits) or flaps of skin (tags). Additionally, affected individuals may have asymmetrical facial features and an unusually small head (microcephaly).
People with Wolf-Hirschhorn syndrome experience delayed growth and development. Slow growth begins before birth, and affected infants tend to have problems feeding and gaining weight (failure to thrive). They also have weak muscle tone (hypotonia) and underdeveloped muscles. Motor skills, such as sitting, standing, and walking, are significantly delayed. Most children and adults with this disorder also have short stature.
Intellectual disability ranges from mild to severe in people with Wolf-Hirschhorn syndrome. Compared to people with other forms of intellectual disability, their socialization skills are strong, while verbal communication and language skills tend to be weaker. Most affected children also have seizures, which may be resistant to treatment. Seizures tend to disappear with age.
Additional features of Wolf-Hirschhorn syndrome include skin changes such as mottled or dry skin, skeletal abnormalities such as abnormal curvature of the spine (scoliosis and kyphosis), dental problems including missing teeth, and an opening in the roof of the mouth (cleft palate) and/or in the lip (cleft lip). Wolf-Hirschhorn syndrome can also cause abnormalities of the eyes, heart, genitourinary tract, and brain.
The reality of the matter is that fetuses with Wolf-Hirschorn syndrome have a high mortality rate. They will either die inside the womb, during childbirth or shortly after.
With a smile on her face and a tear in her eye, she said, “I’m sorry. Bad things happen to good people.” There isn’t a day that goes by that those two sentences in her voice doesn’t go through my head.
At this point, as we call them, the “Team of Doctors” began to assemble; from the infamous Dr. Hummel, the compassionate Dr. Polak and Donna Dorinzi who had the foresight to know when we need space to think or just a quiet comforting hug. Brittany and I sat across the table from many brilliant doctors with only Rilynn’s best interest in mind. We spoke about real life and death issues which WILL impact Rilynn’s and our lives forever. At the time we believed the most difficult portion of this journey was at this point. We, as parents, had a decision to make. Terminate this pregnancy or allow nature to take its course. Please don’t forget the 18 months of trying everything and 2 years of fertility treatments to create the family Brittany and I yearned to have. As parents, we felt it was our duty to provide the best opportunities we could for our unborn child. Terminating the pregnancy would have meant to us that we gave up in the face of adversity. We chose to make the most prudent and well educated decisions we could for Rilynn and allow nature to take its course. Although the Team of Doctors could only guess at the spectrum of issues Rilynn would face, Brittany and I appreciated the open lines of communication from those Doctors. We would rather have all of the information, whether good or bad, than walk blindly through this journey with doctors shaking their heads behind our backs.
Dr. Josh Dower is absolutely the hinge pin to the “Team of Doctors.” We meet Josh approximately 3 weeks prior to her birth and only for about an hour. It took the internet and few people to explain to me what a Pediatric Palliative Care Doctor does and why he was talking to us. In hind sight, the “Team of Doctors” knew what we were going to need. Josh provided us with an open unadulterated way of communicating our feelings. He explained to us that our mixed emotions are normal and we should absolutely “…leave no regrets…”
On September 16, 2010 Brittany’s water had broken high and was unaware it had broken. She had noticed a spot of blood and called the High Risk OB office immediately. Needless to say, she was admitted that evening. Labor was induced around 9pm and the labor and delivery circus began. The fun part was no sleep, family members EVERYWHERE and phone calls to EVERYONE. All of this fun was quietly overshadowed by our fear of our special daughter dying during labor or shortly after. During labor contraction throughout the night, Rilynn’s heart rate would drop. This concerned the High Risk Doctors.
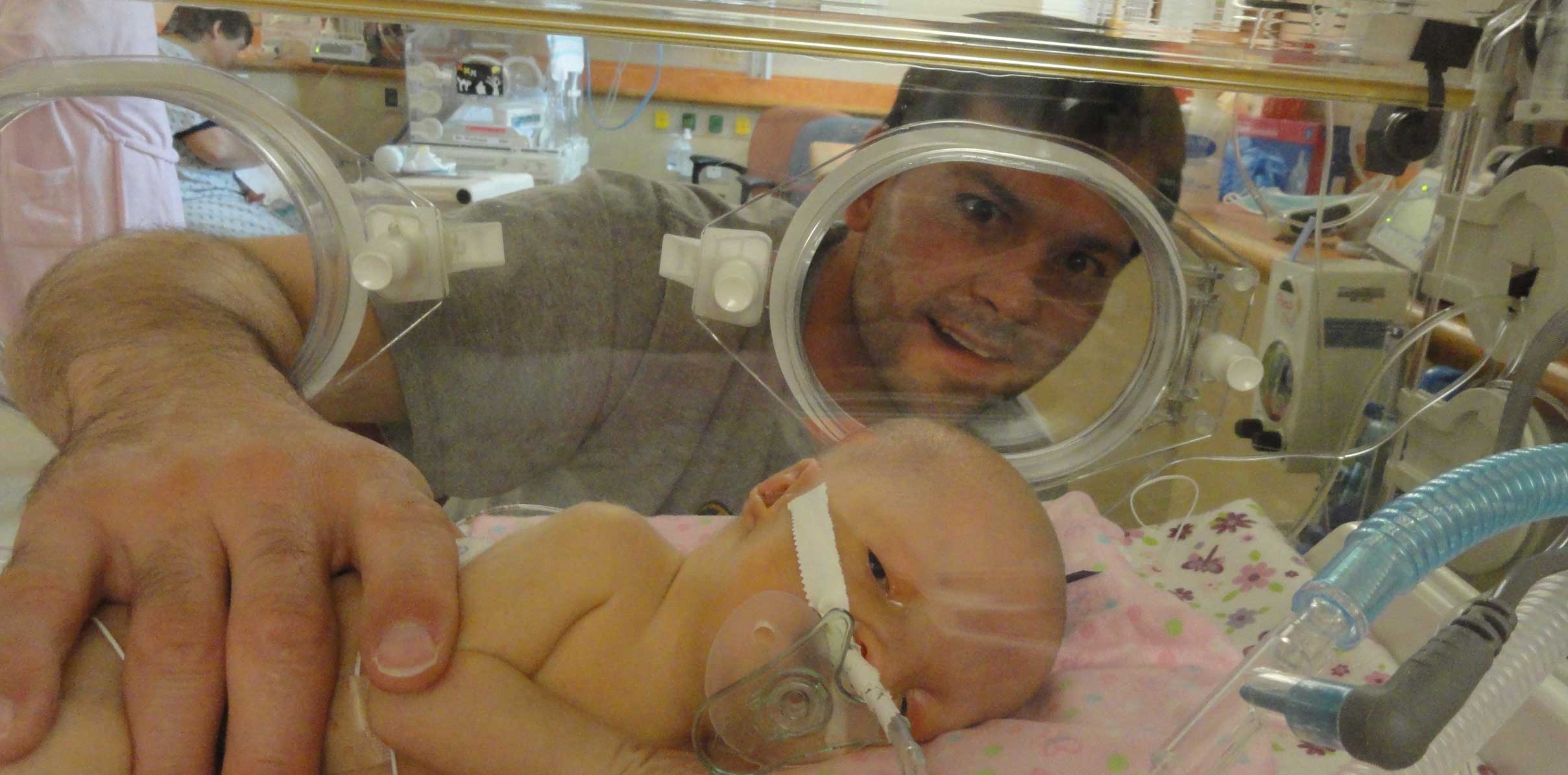
At 8:16 am on September 17, 2010, Rilynn Nicole German arrived into our lives via C-section. I can’t begin to explain how many people from the NICU were there to receive Rilynn into this world. It was a sea of yellow gowns. It felt great to know all of these people were there to honor our wishes and give Rilynn the fighting chance she deserved. We had crossed two HUGE obstacles: not dying in the womb and not dying during child birth. Rilynn was born approximately 6 weeks early weighting under 3 pounds. The NICU team stabilized her and let her rest in the Butterfly room. Our miracle was here.
During the next 6 days, the “Team of Doctors” stopped by and checked in several times. Brittany refused to sleep and would slip out of her hospital room to visit Rilynn in the NICU all night long. I believe the NICU Doctors and Nurses are “Angels from Heaven”. Their compassion and understanding is second to none. They see babies at their worst and frantic parents who place their hearts in their hands. It was a Nurse in the NICU who made the most impact on our lives. Her name is Rebecca Tilly. Rebecca felt that the hospital bedding in Rilynn’s isolette was too scratchy for her. She went to the store on her own time and with her own money purchased receiving blankets to use asbedding. The feeling that Brittany and I had inside when we arrived that morning to visit our baby girl had pink and purple butterfly bedding is unexplainable. Rebecca stepped outside of the box to make sure Rilynn was comfy and we felt like we were not on this island alone.
Every time Rilynn’s heartbeat slowed down or she forgot to breathe the monitor alarms would activate until corrective action was taken. Every time those alarms went off, (they went off a hundred times a day) we thought that was the last second Rilynn had on this earth. Brittany and I took Dr. Dower’s advice and created a journal to chronicle her days, our feelings, sights, sounds and inner thoughts and took over 270 pictures of our experiences.
Just as Brittany and I were starting to allow our nerves to settle down on day six, the midnight phone call we feared from the beginning came. Sometime just prior to 12:00 am on September 23, 2010, Rilynn’s pH levels had begun to rise. Brittany was sleeping at the Ronald McDonald House across the hospital parking lot and I had taken the hour ride home to tend to pending issues. The NICU Nurse called Brittany to inform her Rilynn had taken a turn for the worst. Brittany called me and I was there within an hour and half. I will never forget the tears in the Doctor’s eyes when she came out to give us an update around 3am. Rilynn’s blood pH had become so acidic that it was beginning to breakdown her organs. She had also lost her ability to clot blood. Every time the Doctors and Nurses tried to replace her IVs Rilynn would continue to bleed from that hole. They gave her some blood and cleaned her up so we could see her. I wish I could forget the permanent image I have in my brain of her laying there lifeless with gauze pads the size of her fist taped all over her body and tubes and wires connected all over her. I reached in and placed my hand over body to comfort her and she looked at me and smiled. That was the last smile I saw from my daughter. All I could remember thinking was, “Where is Dr. Dower?” Brittany and I sat next to her isolette with tears in our eyes, an overwhelming fear and an ever so slight feeling of hope. The feelings of hope went away when the sweetest man ever, Dr. Polak, put his hands on our shoulders and whispered in our ears, ”This is Rilynn’s way of telling us she cannot fight anymore. It is time to say good bye.” At that moment, absolutely nothing mattered to Brittany and I but Rilynn. The Doctors and Nurses moved us to a new room where Brittany and I could say good bye alone. Dr. Dower showed up with an encouraging hug while the Nurse removed the breathing tubes and wires so we could hold her for one last time.
At this point, we thought it would be best to list our thoughts and emotions.
Our Emotional Feelings
Elation, Heart dropping, Excitement, Fear, Walking thru the dark, Only ones on the Island, Tears of Joy, Happy, Grief, Worried, Stressful, Invigoration, Confused.
We Appreciate
- All of the Doctors openly communicating good and bad info to us
- Full support by the Team of Doctors of our decision to allow nature take its course
- Team collaboration and research – extremely fast information sharing
- Forward vision to allow meetings with doctors we wouldn’t have never thought of seeking out
- Flexibility in the High Risk OB office’s scheduling to allow for monitoring restricted by our work schedules and travel distance distance.
- Genuine empathy. Not just a smile. Many medical professional put their own hearts into this journey. It felt like they took our hand and walk down the path with us.
We Wish
- The doctors could have guarded us from the gruesome images in the final hours. Catch 22 – We wanted to be there to provide support to our helpless child.
- The doctors would have informed us of the seriousness of Rilynn’s situation prior to “sticking” her several times while trying to find an IV site to administer blood. Clotting and pH issues were already present. We could have saved our current feelings of “Why did we allow them to hurt her when the outcome would have been the same?”
- Dr. Dower would have gotten involved much earlier in our journey. But, he showed up when times were too tough for Brittany and I to handle alone.
Unanswered Questions
- Was there anything we could have done to save her? No MRI? More testing? More persistence from us to push the doctors and nurses to check everything ? ( while IVs were already in and no more pricks were needed)
Although Brittany and I have endured a long journey, we wouldn’t change a decision we made. We do not wish to have our questions answered because the memories and feelings we have are ours forever.
“Unanswered Questions Provide Inspiration”
We love her. We miss her. We are proud of her.
